Have you ever experienced the frightening sensation of wanting to move but being unable to? This phenomenon, known as sleep paralysis, is a peculiar state where the body is temporarily immobilized while the mind remains fully awake. In recent years, researchers have been exploring the intriguing connection between sleep patterns and paralysis, seeking to uncover the mystery behind this puzzling occurrence. Through their efforts, a deeper understanding of this phenomenon has emerged, shedding light on the factors that contribute to sleep paralysis and providing a glimpse into the fascinating world of our sleep patterns.
Sleep Stages
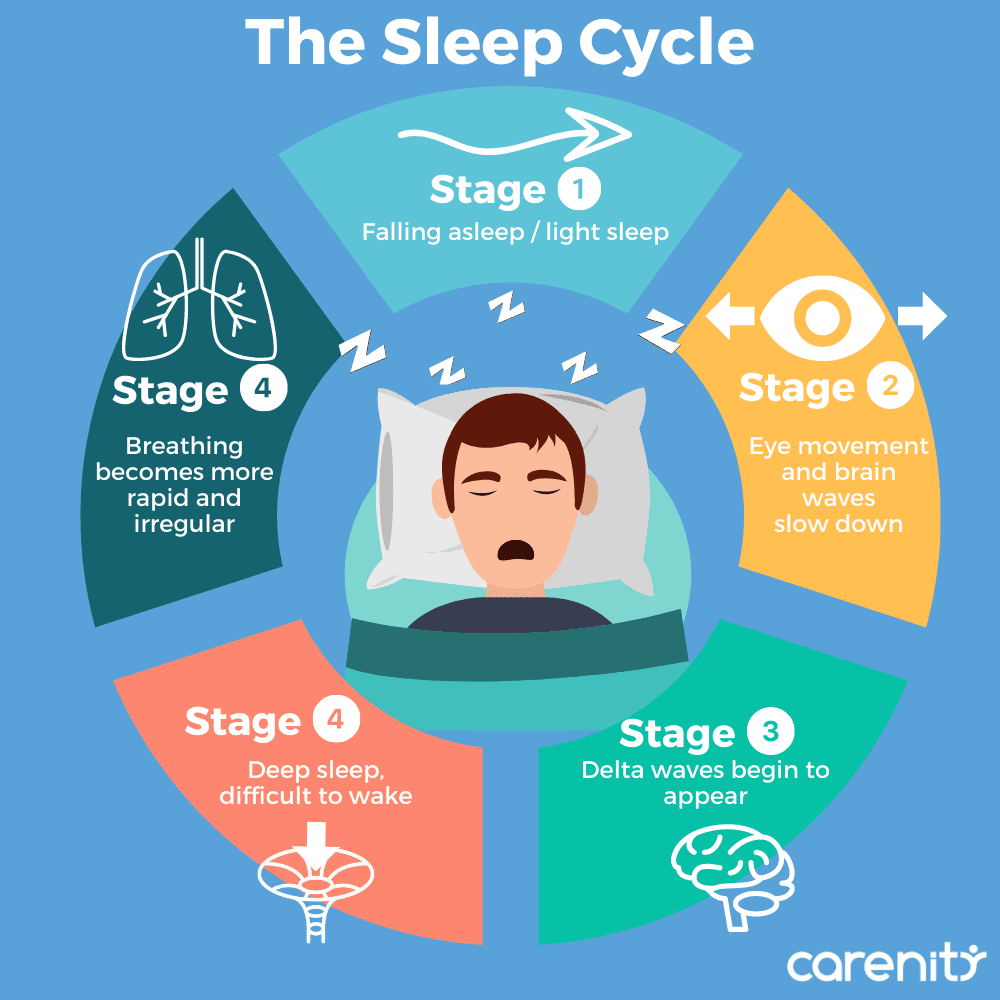
Sleep is comprised of different stages, each with its distinct characteristics and functions. The two main types of sleep are Non-REM (Rapid Eye Movement) sleep and REM sleep. Non-REM sleep can be further divided into three stages – N1, N2, and N3.
Non-REM Sleep
During Non-REM sleep, which typically makes up the majority of your sleep cycle, your body gradually relaxes and enters deeper stages of sleep. In Stage N1, you are in a light sleep, easily awakened by external stimuli. This stage is often characterized by slow eye movements and may last only a few minutes.
As you progress to Stage N2, your heart rate and breathing continue to slow down, and your body temperature drops. This is the stage where your body prepares for the deep sleep in Stage N3.
Stage N3, also known as slow-wave sleep or deep sleep, is the stage in which your body repairs and rejuvenates itself. Your blood pressure drops, and your muscles relax even further. This stage is crucial for physical restoration, and if you are deprived of deep sleep, you may wake up feeling groggy and unrested.
REM Sleep
REM sleep, on the other hand, is the stage in which most vivid dreaming occurs. It is characterized by rapid eye movements and increased brain activity. During REM sleep, your brain consolidates memories and processes emotions. Your muscles become temporarily paralyzed to prevent you from acting out your dreams.
It is important to note that sleep paralysis often occurs during the transition in and out of REM sleep, when the brain is awake, but the body remains immobile. This phenomenon can be both perplexing and frightening, but it is essential to understand that sleep paralysis is generally harmless.
Sleep Paralysis
Definition
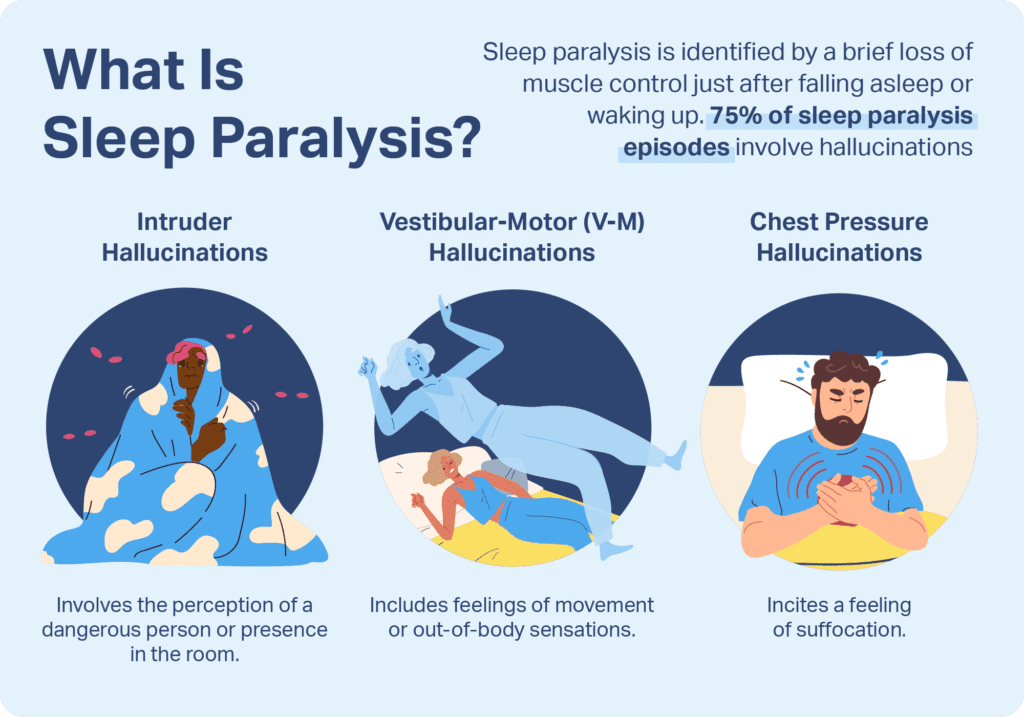
Sleep paralysis is a temporary inability to move or speak that occurs while falling asleep or waking up. During an episode of sleep paralysis, you may be fully conscious but unable to move your body or speak. It is often accompanied by hallucinations and a sense of pressure on the chest.
Causes
Sleep paralysis is primarily caused by a disruption in the normal transition between sleep stages, specifically the transition between wakefulness and REM sleep. When this transition is disturbed, the brain may become alert while the body remains in a state of paralysis.
Several factors can contribute to the occurrence of sleep paralysis. These include sleep deprivation, irregular sleep schedules, sleep disorders such as narcolepsy or sleep apnea, and certain medications.
Symptoms
The main symptom of sleep paralysis is the temporary inability to move or speak. Other common symptoms include a feeling of pressure on the chest, hallucinations (both auditory and visual), and a sense of impending doom or a malevolent presence.
Sleep paralysis episodes can last from a few seconds to a few minutes, and they generally end spontaneously or when the person is startled awake by a noise or physical touch.

Sleep Disorders Associated with Paralysis
Narcolepsy
Narcolepsy is a sleep disorder characterized by excessive daytime sleepiness and sudden, uncontrollable episodes of falling asleep. Sleep paralysis is a common symptom experienced by individuals with narcolepsy, often occurring alongside other symptoms such as cataplexy (sudden loss of muscle tone) and hallucinations.
Sleep Apnea
Sleep apnea is a sleep disorder characterized by pauses in breathing during sleep. These pauses can last for several seconds and occur multiple times throughout the night, leading to disruptions in sleep. Sleep apnea has been linked to an increased risk of sleep paralysis, as the interruptions in breathing can trigger abnormal sleep transitions.
Insomnia
Insomnia is a sleep disorder characterized by difficulty falling asleep, staying asleep, or experiencing non-refreshing sleep. While sleep paralysis is not directly caused by insomnia, individuals with insomnia may be at a higher risk due to the disruptions in sleep patterns and the potential for sleep deprivation.
Circadian Rhythm and Paralysis
The Role of Circadian Rhythm
The circadian rhythm is a natural, internal process that regulates the sleep-wake cycle in humans. It is influenced by external factors such as light and darkness and plays a crucial role in determining the timing of sleep and wakefulness.
Disruptions to the circadian rhythm, such as those caused by shift work or frequent time zone changes, can negatively impact sleep patterns and increase the likelihood of sleep paralysis episodes.
Shift Work and Paralysis
Shift work, particularly night shifts, can disrupt the natural sleep-wake cycle and result in irregular sleep patterns. This can lead to a higher occurrence of sleep paralysis episodes and an increased risk of sleep disorders.
Jet Lag and Paralysis
Jet lag occurs when you rapidly travel across multiple time zones, causing a misalignment between your internal circadian rhythm and external time cues. Jet lag can result in disrupted sleep patterns, leading to an increased susceptibility to sleep paralysis during the adjustment period.
Sleep Paralysis as a Symptom of Other Conditions
Anxiety and Stress
High levels of anxiety and stress can disrupt sleep patterns and contribute to the occurrence of sleep paralysis. The hormonal changes associated with stress can affect the brain’s ability to regulate sleep transitions properly, leading to an increased risk of sleep paralysis episodes.
Narcolepsy
As mentioned earlier, sleep paralysis is a common symptom of narcolepsy. Individuals with narcolepsy may experience sleep paralysis during the daytime, often triggered by emotional stress or sleep deprivation.
Sleep Disorders
Various sleep disorders, such as insomnia, sleep apnea, and restless leg syndrome, can increase the likelihood of sleep paralysis episodes. The disruptions in sleep caused by these disorders can lead to abnormal sleep transitions and a higher risk of experiencing sleep paralysis.
Mental Health Conditions
Certain mental health conditions, such as depression and post-traumatic stress disorder (PTSD), have been associated with an increased risk of sleep paralysis. The exact mechanisms behind this connection are not fully understood, but it is believed that the disruptions in neurotransmitters and brain activity related to these conditions may contribute to the occurrence of sleep paralysis.
Sleep Paralysis Treatments
Improved Sleep Hygiene
Practicing good sleep hygiene is crucial for maintaining healthy sleep patterns and reducing the occurrence of sleep paralysis. This includes establishing a regular sleep schedule, creating a comfortable sleep environment, avoiding stimulating activities before bed, and limiting the consumption of caffeine and alcohol.
Medications
In some cases, medications may be prescribed to manage sleep paralysis and any underlying sleep disorders or mental health conditions. These medications may include antidepressants, anti-anxiety drugs, or medications specifically targeting sleep disorders such as narcolepsy or sleep apnea. It is important to consult with a healthcare professional to determine the best course of action for your specific situation.
Therapies
Various therapies, such as cognitive-behavioral therapy for insomnia (CBT-I) or exposure therapy for anxiety, can be beneficial in managing sleep paralysis. These therapies aim to address the underlying causes and triggers of sleep paralysis, helping individuals develop healthier sleep patterns and coping mechanisms.

Tips for Managing Sleep Paralysis
Maintaining a Regular Sleep Schedule
Establishing a consistent sleep schedule, including regular bedtimes and wake-up times, can help regulate your sleep patterns and reduce the occurrence of sleep paralysis. This consistency reinforces your body’s internal clock and promotes more restful sleep.
Creating a Relaxing Sleep Environment
Designing a sleep environment that is conducive to relaxation and sleep can also contribute to managing sleep paralysis. This includes keeping the bedroom cool, dark, and quiet, using comfortable bedding and pillows, and creating a calming nighttime routine before bed.
Stress Management Techniques
Developing effective stress management techniques can be helpful in reducing the frequency and intensity of sleep paralysis episodes. Techniques such as deep breathing exercises, meditation, yoga, and journaling can all help alleviate stress and promote better sleep.
Research and Studies on Sleep Paralysis and Sleep Patterns
Current Understanding and Hypotheses
Researchers continue to investigate the underlying mechanisms of sleep paralysis and its relationship to sleep patterns. Current theories suggest that disruptions in sleep stages, particularly the transition between wakefulness and REM sleep, play a crucial role in the occurrence of sleep paralysis. However, further research is still needed to fully understand and explain this phenomenon.
Experimental Studies
Experimental studies have been conducted to explore the effects of sleep deprivation, sleep fragmentation, and various sleep disorders on sleep paralysis. These studies involve monitoring brain activity, sleep stages, and physiological responses during sleep to gain insights into the triggers and mechanisms of sleep paralysis.
Observational Studies
Observational studies have also been conducted to examine the prevalence and characteristics of sleep paralysis in different populations. These studies aim to identify potential risk factors, such as age, gender, and psychological disorders, and provide a broader understanding of the connections between sleep paralysis and sleep patterns.
The Impact of Sleep Patterns on Daily Life
Work Performance
Disrupted sleep patterns, including those associated with sleep paralysis, can have a significant impact on work performance. Sleep deprivation and poor sleep quality can lead to decreased cognitive function, reduced concentration, and impaired decision-making abilities, ultimately affecting productivity and job performance.
Mental Health
Healthy sleep patterns are crucial for maintaining good mental health. Disrupted sleep, including sleep paralysis episodes, can contribute to the development or aggravation of mental health conditions such as depression and anxiety. On the other hand, improving sleep patterns can enhance emotional well-being and overall mental health.
Physical Health
Sleep plays a vital role in physical health and is essential for cellular repair, immune function, and hormone regulation. Disruptions in sleep patterns, including those related to sleep paralysis, can have adverse effects on physical health, increasing the risk of chronic conditions such as cardiovascular disease, obesity, and diabetes.
Conclusion
Understanding the connection between sleep patterns and paralysis is crucial for managing sleep paralysis and maintaining overall well-being. By prioritizing healthy sleep habits, seeking appropriate treatment for underlying sleep disorders or mental health conditions, and implementing stress management techniques, you can minimize the occurrence and impact of sleep paralysis episodes. Remember, sleep paralysis is generally harmless, and with the right strategies, you can improve your sleep patterns and enjoy restful nights.
