Have you ever experienced the unsettling sensation of being unable to move or speak when you wake up from sleep? This phenomenon is known as sleep paralysis, and it can be a terrifying experience. But did you know that sleep paralysis has been linked to depression? In this article, we will explore the connection between sleep paralysis and depression, and what you need to know about this fascinating and often misunderstood topic.

What is sleep paralysis?
Definition
Sleep paralysis is a phenomenon that occurs during the transition between sleep and wakefulness. It is characterized by a temporary inability to move or speak, accompanied by a feeling of being paralyzed. This phenomenon usually lasts a few seconds to a few minutes, but it can be a distressing and terrifying experience for those who have never encountered it before.
Symptoms
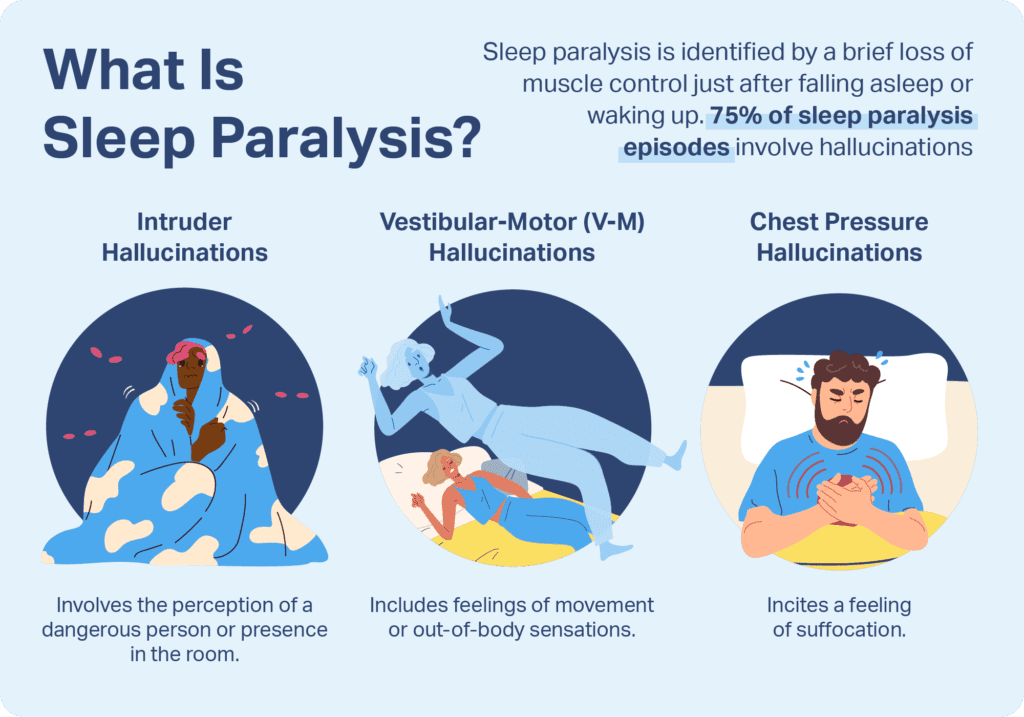
During an episode of sleep paralysis, you may experience the inability to move any part of your body, despite being mentally awake and aware of your surroundings. This can be accompanied by vivid hallucinations, such as seeing shadows or figures in the room, feeling a presence, or hearing strange noises. Additionally, individuals may also report a feeling of pressure on their chest or difficulty breathing.
Causes
The exact cause of sleep paralysis is still not fully understood, but it is believed to be related to disruptions in the sleep cycle. Sleep paralysis often occurs during the rapid eye movement (REM) stage of sleep, when dreaming takes place. During this stage, the brain sends signals to temporarily immobilize the muscles in order to prevent us from acting out our dreams. In sleep paralysis, however, this muscle relaxation continues even after waking up, leading to the feelings of being unable to move.
Link between sleep paralysis and depression
Prevalence of sleep paralysis in individuals with depression
Research has shown a strong association between sleep paralysis and depression. In fact, individuals with depression are more likely to experience sleep paralysis compared to the general population. Studies have found that up to 50% of individuals with depression have reported experiencing sleep paralysis at some point in their lives.
Effect of sleep paralysis on depression symptoms
Sleep paralysis can have a significant impact on the symptoms of depression. Episodes of sleep paralysis can disrupt sleep patterns and lead to poor sleep quality, which in turn can worsen depression symptoms such as fatigue, low mood, and difficulty concentrating. The fear and anxiety associated with sleep paralysis episodes can also contribute to feelings of helplessness and hopelessness, further exacerbating depressive symptoms.
Role of depression in the development of sleep paralysis
While sleep paralysis can occur independently of any mental health conditions, there is evidence to suggest that depression may play a role in the development of sleep paralysis. It is believed that the disruptions in sleep patterns and the hyper-arousal state commonly experienced by individuals with depression may increase the likelihood of experiencing sleep paralysis.
Impact of sleep paralysis on mental health
Anxiety and stress
Sleep paralysis can be an incredibly distressing experience, often causing feelings of anxiety and stress. The inability to move or speak, combined with the presence of hallucinations, can create a sense of fear and panic. This heightened emotional state can then spill over into daily life, leading to increased feelings of anxiety and stress.
Quality of life
The frequent occurrence of sleep paralysis can significantly impact one’s quality of life. Individuals may develop a fear of falling asleep due to the anticipation of experiencing sleep paralysis. This fear can result in sleep disturbances, leading to daytime fatigue, difficulty concentrating, and impaired functioning in various aspects of life, including work and relationships.
Psychological impact
Sleep paralysis can have profound psychological effects on individuals. The terrifying hallucinations and feelings of helplessness associated with sleep paralysis can cause distress, leading to increased vulnerability to other mental health issues such as anxiety disorders and mood disorders. Moreover, the psychological impact can further perpetuate the cycle of sleep disturbances and negative emotional states.
Managing sleep paralysis and depression
Seeking professional help
If you are experiencing sleep paralysis and depression, it is crucial to seek professional help. A mental health professional, such as a therapist or psychiatrist, can provide guidance and support in managing both sleep paralysis and depression. They can help you understand the underlying causes and develop individualized treatment plans to address your specific needs.
Practicing good sleep hygiene
Establishing a consistent sleep routine and practicing good sleep hygiene can greatly improve sleep quality and help reduce the incidence of sleep paralysis. This may include maintaining regular sleep and wake times, creating a comfortable sleep environment, avoiding stimulants like caffeine and electronics before bed, and engaging in relaxation techniques before sleep.
Stress management techniques
Stress can exacerbate both sleep paralysis and depression symptoms. Learning and implementing effective stress management techniques can help alleviate the impact of stress on sleep and mood. Techniques such as deep breathing exercises, mindfulness meditation, and engaging in enjoyable hobbies or activities can help reduce stress levels and promote better sleep.
Other sleep disorders and depression
Insomnia and depression
Insomnia, a sleep disorder characterized by difficulty falling asleep or staying asleep, is commonly associated with depression. The presence of insomnia can increase the risk of developing depression, and in turn, depression can worsen insomnia symptoms. Managing insomnia through similar treatment approaches as sleep paralysis, such as cognitive-behavioral therapy and good sleep hygiene, can have a positive impact on both sleep and mood.
Sleep apnea and depression
Sleep apnea, a condition characterized by pauses in breathing during sleep, has also been linked to depression. The disrupted sleep caused by sleep apnea can result in excessive daytime sleepiness, irritability, and decreased quality of life, which can contribute to depressive symptoms. Treatment options for sleep apnea, such as continuous positive airway pressure (CPAP) therapy, can improve sleep and alleviate depression symptoms.
Narcolepsy and depression
Narcolepsy, a neurological disorder characterized by excessive daytime sleepiness and sudden loss of muscle control (cataplexy), has been associated with an increased risk of depression. The impact of narcolepsy on daily functioning, along with the disruptions in sleep-wake cycles, can contribute to depressive symptoms. Treating narcolepsy with medications and lifestyle modifications can improve symptoms and potentially alleviate depressive episodes.
Tips for coping with sleep paralysis
Educating oneself about sleep paralysis
Understanding the nature and causes of sleep paralysis can help demystify the experience and reduce anxiety surrounding it. Learning about the factors that contribute to sleep paralysis, such as disruptions in the sleep cycle, can empower individuals to better manage and cope with episodes when they occur.
Developing a routine sleep schedule
Establishing a regular sleep schedule, where you go to bed and wake up at the same time every day, can help regulate your sleep-wake cycle. This consistency can promote better sleep quality and reduce the likelihood of experiencing sleep paralysis. Additionally, creating a relaxing bedtime routine and ensuring a comfortable sleep environment can further enhance your sleep routine.
Creating a comfortable sleep environment
Designing a sleep environment that promotes relaxation and comfort can contribute to better sleep and reduce the frequency of sleep paralysis episodes. Ensuring that your sleep environment is quiet, dark, and cool can help create the ideal conditions for sleep. Additionally, investing in a comfortable mattress, pillows, and bedding can also improve sleep quality and reduce physical discomfort that may contribute to sleep paralysis.

Understanding the sleep cycle
Stages of sleep
Sleep is divided into several stages, each with its own distinct characteristics. These stages include wakefulness, non-rapid eye movement (NREM) sleep, and rapid eye movement (REM) sleep.
REM sleep
Rapid eye movement (REM) sleep is a stage of sleep marked by rapid eye movements, vivid dreams, and muscle paralysis. It is during this stage that sleep paralysis most commonly occurs. The brain is highly active during REM sleep, and the body experiences temporary muscle atonia to prevent acting out dreams.
Relation between sleep stages and sleep paralysis
Sleep paralysis is most likely to occur during the transition between REM sleep and wakefulness. This is because the brain is still in a state of muscle paralysis associated with REM sleep, even though the individual has become mentally awake. The disruption in the normal sleep-wake cycle can result in the temporary inability to move or speak.
Recognizing the signs of depression
Symptoms of depression
Depression is a complex mental health condition that can manifest in various ways. Common symptoms of depression include persistent sadness, lack of interest or pleasure in activities, changes in appetite and weight, sleep disturbances, fatigue, feelings of guilt or worthlessness, difficulty concentrating, and thoughts of death or suicide. It is important to recognize these signs and seek professional help if you or someone you know is experiencing them.
Seeking professional help
If you suspect that you or someone you know may be experiencing depression, it is essential to seek professional help. A healthcare provider or mental health professional can evaluate symptoms, provide an accurate diagnosis, and develop a comprehensive treatment plan. Early intervention and appropriate treatment are crucial in managing depression and reducing its impact on daily life.
Supportive measures
In addition to seeking professional help, it is important to have a support system in place. Sharing your feelings and experiences with trusted friends or family members can help alleviate the emotional burden of depression. Support groups and online communities can also provide a valuable source of understanding and guidance from individuals who have faced similar challenges.

Possible treatment options
Cognitive-behavioral therapy (CBT)
Cognitive-behavioral therapy (CBT) is a widely recognized and effective treatment for both sleep disorders and depression. CBT aims to identify and change negative thought patterns and behaviors that contribute to sleep disturbances and depressive symptoms. By addressing maladaptive thinking and implementing healthy coping strategies, CBT can help individuals manage sleep paralysis and improve their overall mental well-being.
Pharmacological interventions
Medications may be prescribed to help manage the symptoms of depression and sleep disturbances, including sleep paralysis. Antidepressants, such as selective serotonin reuptake inhibitors (SSRIs) or tricyclic antidepressants (TCAs), can help regulate mood and improve sleep patterns. However, it is important to consult with a healthcare professional to determine the most appropriate medication and dosage for your specific needs.
Complementary and alternative therapies
Complementary and alternative therapies, such as acupuncture, yoga, and mindfulness-based practices, have been found to be beneficial in managing both sleep disorders and depression. These approaches can help promote relaxation, reduce stress levels, and improve overall well-being. It is important to discuss these options with a healthcare professional and ensure their integration into a comprehensive treatment plan.
Conclusion
Promoting awareness and understanding of the link between sleep paralysis and depression is crucial in providing support and effective management strategies for individuals who experience these conditions. Sleep paralysis can have a significant impact on mental health, causing increased anxiety, decreased quality of life, and potential psychological distress. By seeking professional help, practicing good sleep hygiene, and employing stress management techniques, individuals can better cope with sleep paralysis and its association with depression. Taking a holistic approach to managing these conditions, including understanding the sleep cycle and recognizing the signs of depression, can lead to improved overall mental health and well-being. Remember, you don’t have to face sleep paralysis and depression alone – help is available!


